DEFINITIONS OF COMMONLY USED TERMS
1. Sequential Intercept Model
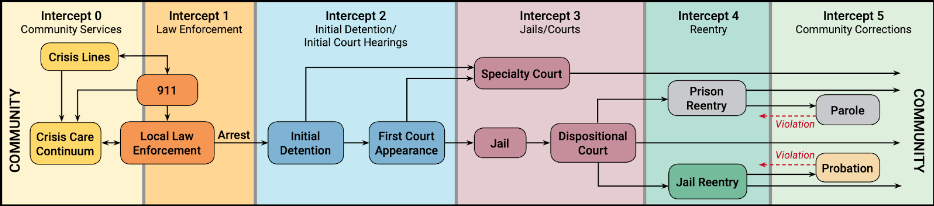
Abreu, D. Parkter, T.W., Noether, C.D., Steadman, H.J., & Case, B. (2017). Revising the paradigm for jail diversion fro people with mental and substance use disorders: Intercept O. Behavioral Sciences & the Law, 35(5-6), 380-395, https://doi.org/10.1002/bsl.2300
@2019 Policy Research Associates, Inc.
The Sequential Intercept Model, developed in the early 2000s, is a tool to identify points when people with mental health or substance use concerns can be “intercepted” in order to provide them with treatment or support services and to help them avoid entry to or deeper involvement in the criminal justice system. It allows communities to assess resources, determine gaps in services, and design programs to benefit persons who need treatment or social support. Each intercept level can be imagined as a filter: without strong cross-sector partnerships, substance use may not be detected or treated.
According to Munetz and Griffin, who created the tool, the intercept model has several objectives: preventing involvement in the criminal justice system, reducing jail admissions, engaging people in treatment as soon as possible, minimizing time spent moving through the criminal justice system, linking people to community treatment upon release from incarceration, and reducing returns to the criminal justice system.
Many partners in the Opioid Collaborative are using the Sequential Intercept Model as a framework for identifying issues and developing interventions, as well as to identify which community partners to involve.
Sources:
2. High-utilizers
This term typically refers to people who have frequent contact with services or systems that are not intended for regular use and where regular use signals social or medical issues that are unresolved or better addressed by other means. These services and systems might include the emergency room, child welfare response, or the criminal justice system. Typically, addressing needs in this way is costly and ineffective.
Interventions that focus on high utilizers can help these individuals address their healthcare and other needs in a stable, sustainable way. These interventions free up a disproportionately large amount of resources per person successfully treated.
Similar terms include “frequent flier” or “super utilizer,” which are also also used in some criminal justice and healthcare settings to describe a similar phenomenon. Another term for this population with less stigma is familiar faces, coined by public health professionals in Seattle.
Sources:
-
University of Pennsylvania. Targeting High Utilizers of Health Care.
-
Advisory Board. How Kaiser is reaching out to 'super-utilizers.'
3. Opioid Use Disorder
Opioid Use Disorder, or OUD, is a medical term that describes a pattern of opioid use that leads to serious impairment or distress.
The Diagnostic and Statistical Manual of Mental Disorders, which is the leading diagnostic tool used in the United States, defines specific criteria to determine if a person has a substance use disorder. To be diagnosed with OUD, a person must have two or more specified symptoms within a 12-month period. These include cravings, interference with work or family life, and withdrawal. OUD can be classified as mild, moderate, or severe, depending on how many symptoms a person experiences.
Sources:
4. Medication-Assisted Treatment (MAT)
Medication-Assisted Treatment (MAT) is the use of medications with counseling and behavioral therapies to treat substance use disorders and prevent opioid overdose.
There are two main types of drugs used in MAT: agonists, which bind to and activate opioid receptors, and antagonists, which block agonists from binding to receptors.
Agonists, like buprenorphine and methadone, are opioids. They bind to opioid receptors, eliminate withdrawal symptoms, and relieve cravings. Agonists are typically prescribed to people who still have opioids in their system and have not detoxed.
Antagonists, such as naltrexone (Vivitrol), are typically administered via slow-release injection. Antagonists completely block opioids from binding to receptors, and should be prescribed only once a person has fully detoxed; otherwise, the drug causes uncomfortable withdrawal symptoms. Even if the client has fully detoxed, they may not feel well after receiving Vivitrol injections. This is because the blocking function can also block normal dopamine receptors, resulting in feelings of depression (research on this effect is inconclusive).
There are also “partial agonist” and “agonist-antagonist” drugs on the market that have combined effects, and that are available in both pill and extended-release form. Suboxone is one example recently approved by the FDA.
Sources:
